Patient Management Billing Operating System
Screenshot 1.
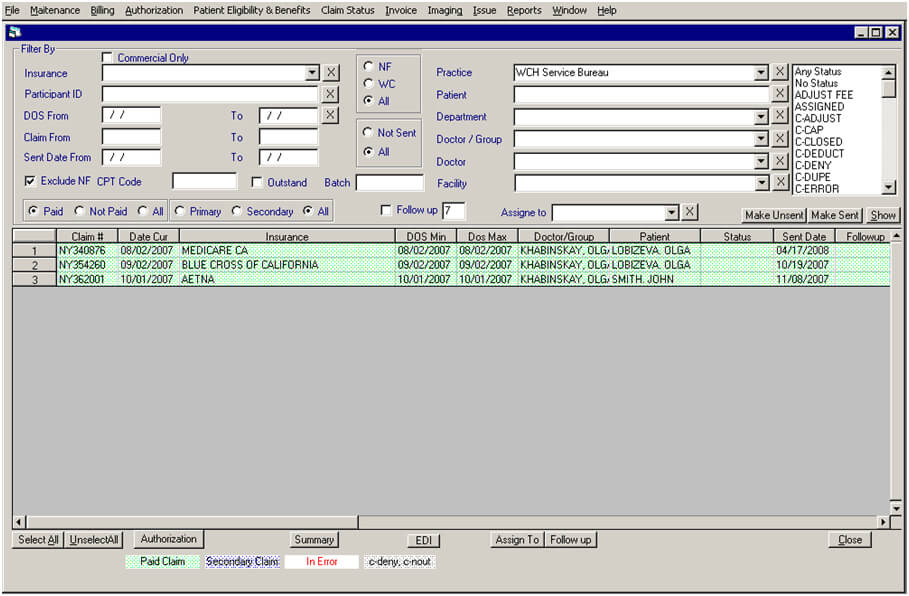
Main page: work with claims. This page is used to work with all claims of practices. You can use different filters to find those claims you would like to work with. You can sort claims by practice name, status, date of service, date of submission, insurance name, health plan, paid or not paid and primary as well as secondary claims. When you chose the necessary filters and click "Show," all claims that match the criteria are then displayed in the main window. For example (as shown on the screenshot) Filters: Practice name (WCH Service Bureau), Paid claims, All (primary and secondary) there are displayed 3 claims for Dr. Khabinskaya (this Dr is working under group WCH Service Bureau), with 2 different patients (2 claims for one patient and 1 for another). All billed claims have their claim# starts with NY… You can find specific claim by entering claim# (for example NY340876) in box Claim from.
Screenshot 2.
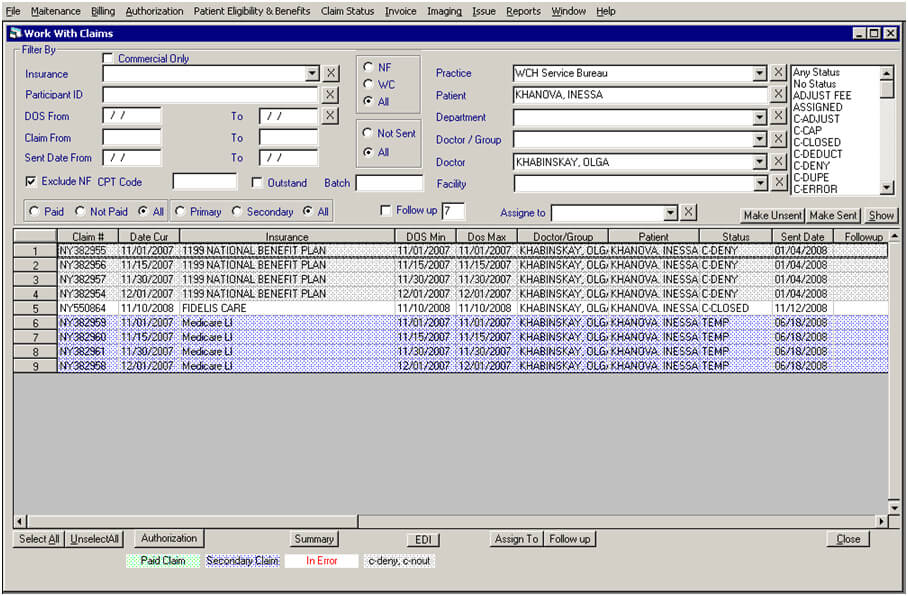
Main page: work with claims. This is the same window as on screenshot 1. There are displayed claims for one patient billed under group WCH Service Bureau and under Dr. Khabinskaya. All claims have their color. Green means paid claim, blue means secondary claim(patient has more than one insurance, and creates when primary is paid), grey means closed claim which was denied and cannot be reprocessed for payment, white means claim is still in process and must be worked out. You can also use this page to create an EDI file or to select claims and send them to insurance companies for payment.
Screenshot 3.
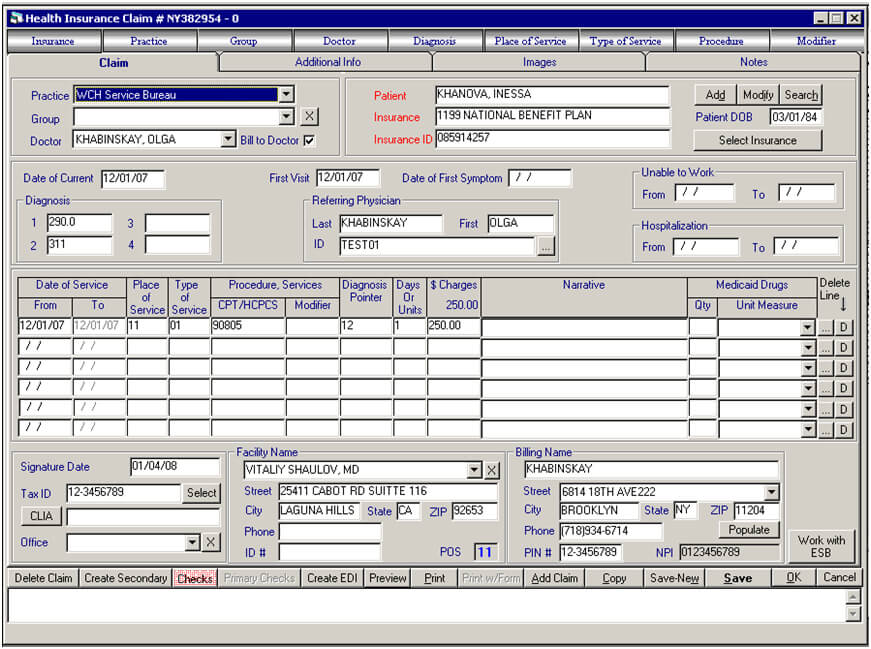
Claim Form interface. Use this form to create claims for the selected practice or provider, under the chosen patient. This claim form displays all of the information about the service that was provided for the patient on the exact date by the physician. . There are also patient’s insurance information, insurance ID number, diagnosis and procedure codes which were billed. At the bottom of claim form there is all information for provider, including Tax ID, NPI, PIN, billing and service addresses.
Screenshot 4.
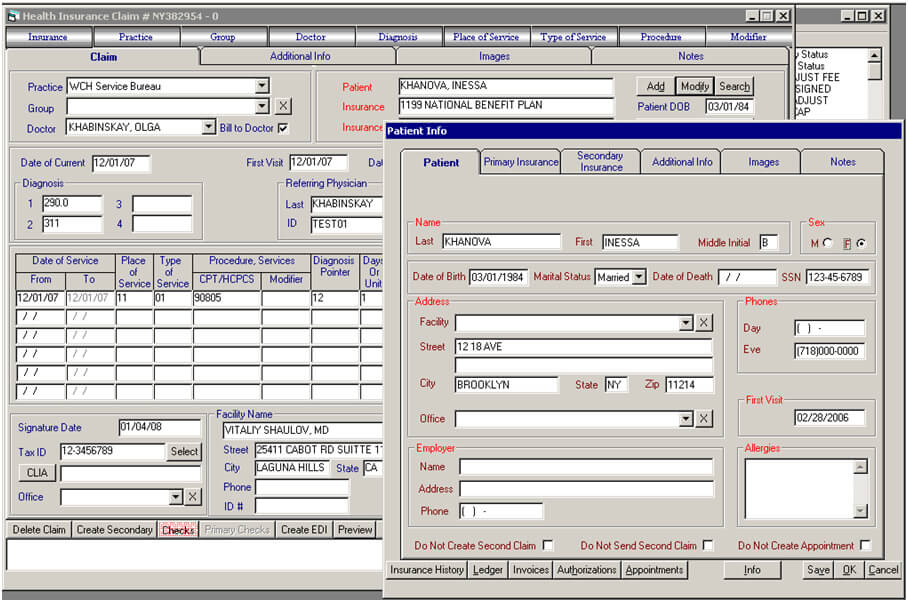
Patient information inlay inside of the claim form. To enter information for a new patient click "Add" the in claim form. To see information for existing patient, click "Modify" in the claim form. There are 6 inlays. Inlay “patient” includes all personal information for the patient, such as their last and first name, sex, date of birth, marital status, SSN number, home address, phone number and employer. Second and third inlay includes patient’s insurance information, for instance, the name of the insurance company, their ID number, effective and termination date, policy holder information along with an address for claim submission. Others inlays are for any additional patient information.
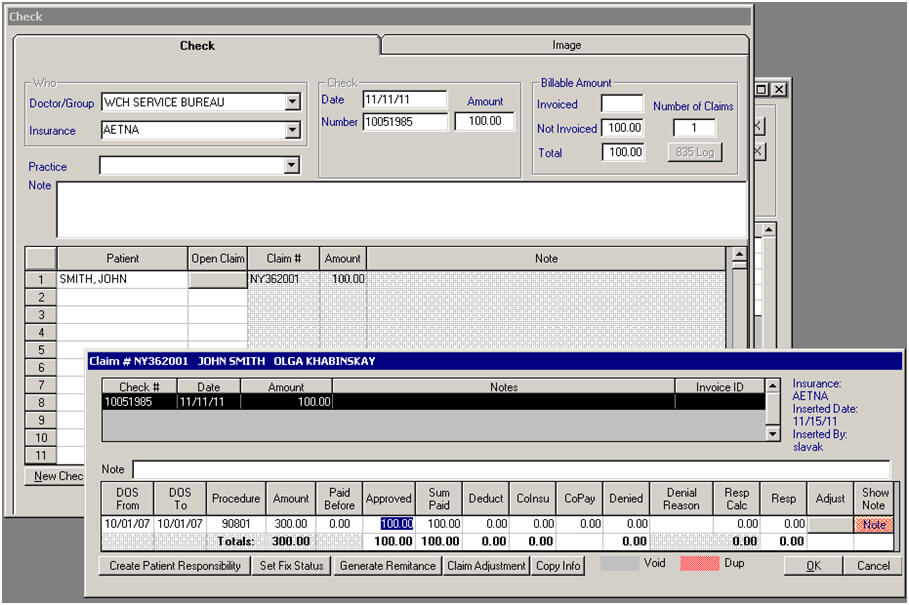
Screenshot 5.
Payment information page. When claims are paid, an Explanation of Benefits is received from the insurance company. We are using this page to enter payment information in the PMBOS program. To open this window, you must first click on the "Work with claims" and select at the top" Billing and Payment." A new window will then be displayed. In this window, there is information regarding payment such as where the insurance payment was received from, under which provider and the check number along with the total amount. You must then enter claims that were processed for payment under this check. Claims are submitted under their number and are sent from New York. Within these claims, payment information is included such as how much was approved, how much was paid, if the patient must pay extra and adjustment codes. After payment was entered, claim becomes green in work with claims. The invoice can then be created and sent to the provider for payment.



